Pain Management: Understanding Types of Pain and Finding What Works
Managing pain at home can feel confusing and scary. You may worry about taking too much and causing harm — or taking too little and not getting relief. Understanding exactly when and how to take your pain medication according to your provider’s orders is critical. In this post, we’ll cover why pain medications are prescribed, the types of pain, medication options, timing, safety tips, non-medication strategies, and how expert nursing support can help you stay safe and comfortable at home.
Understanding Different Types of Pain and What Helps Them
Pain isn’t one-size-fits-all — the type of pain you experience often determines which treatments will help the most. Understanding this can help you and your healthcare provider choose the right treatment, reduce confusion, improve relief, and keep you safer at home.
-
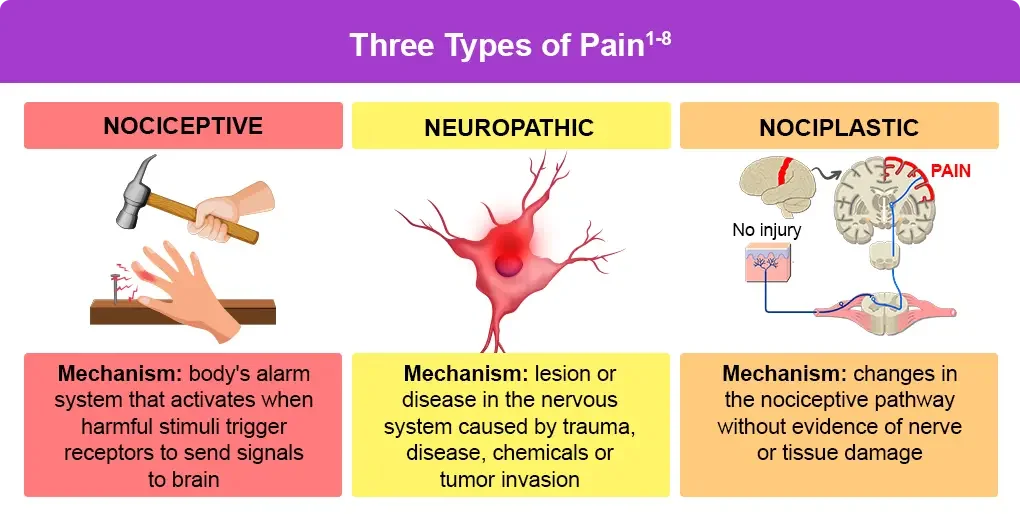
Pain from actual injury or physical stress on the body. Usually sharp, aching, or throbbing.
Examples: Pain from a recent surgery, a broken bone, arthritis (wear-and-tear pain in joints), or repetitive strain injuries. -
Pain caused by nerve irritation or damage. Often described as burning, tingling, or electric shocks.
Examples: Nerve pain from diabetes (diabetic neuropathy), shingles, or nerve compression from spinal problems. -
Pain that occurs when the nervous system becomes more sensitive, even without a clear injury. Often feels widespread or persistent.
Examples: Fibromyalgia, chronic headaches, or general body aches that linger long after an illness or injury. -
Pain that combines more than one type, such as injury-based pain plus nerve or sensitivity pain.
Examples: Cancer-related pain that includes tissue and nerve components, post-surgical pain with lingering nerve irritation, or chronic arthritis pain with burning or tingling sensations.
Reference: Ballantyne JC, Mao J. Opioid Therapy for Chronic Pain. NCBI PMC. 2003; https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11513809/
Why Pain Medication is Prescribed
Pain medications are prescribed to help you recover, reduce discomfort, and improve quality of life. They may be recommended after surgery, for chronic conditions, or to manage acute injuries. Taking medications exactly as directed ensures your pain is controlled without causing unnecessary harm.
Types of Pain Medications and How They Work
Pain medications come in several forms, and each works differently in the body:
Oral medications – Pills, capsules, liquids
Topical patches – Applied to skin, releasing medication over hours or days
Other forms – Injections, creams, or specialty medications
Important: The timing, type, and dose of your medication must always follow your provider’s orders. Never adjust your dose without consulting them.
Timing and Frequency:
Pain medications are often scheduled at specific intervals:
Typically every 4, 6, or 8 hours for oral medications
Patches may release medication over 24–72 hours
Proper spacing ensures steady pain control and reduces risks such as overdose or insufficient relief.
Why Proper Spacing Matters
Following your provider’s instructions helps maintain consistent pain relief and reduces the risk of complications. Never self-dose additional pills if your pain feels severe unless explicitly instructed by your provider. Misuse can lead to serious or life-threatening effects.
Non-Medication Strategies for Pain Relief
Medications are only one part of pain management. Non-pharmacological methods can complement medication and help reduce long-term pain, especially for chronic conditions.
For Chronic Low Back Pain
Aerobic exercise: walking, swimming, cycling
Water exercises: gentle movement to reduce joint stress
For Neck Pain
Yoga or tai chi: improves posture, flexibility, and muscle strength
Gentle stretching and mobility exercises
Reference: Cherkin DC, et al. Non-pharmacological interventions for chronic musculoskeletal pain. NCBI PMC. 2002; https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11866493/
Preventing Side Effects and Recognizing Danger Signs
Even when taken correctly, pain medications can cause side effects. Here are tips to stay safe:
Constipation: Drink plenty of water, eat fiber, and move as advised
Drowsiness or impaired driving: Avoid driving or operating machinery
Life-threatening signs: Monitor breathing, alertness, and overall responsiveness. Do not administer medication if the patient is confused or declining; seek immediate medical help
Caregivers play a crucial role in monitoring for changes in mentation and respiratory function.
How Regal Rejuvenation Can Help
Our experienced nurses provide in-home medication management and discharge support, ensuring all medications are administered safely and effectively according to provider orders. We follow evidence-based guidelines from organizations such as:
National Council of State Boards of Nursing (NCSBN)
California Board of Nursing (BON)
With Regal Rejuvenation, patients in Los Angeles County and surrounding areas can feel confident their pain medications are managed safely.
For more information on supporting health at home, check out our [Chronic Disease Management blog] and [Medication Management] for additional tips.
References
Ballantyne JC, Mao J. Opioid Therapy for Chronic Pain. NCBI PMC. 2003; https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11513809/
Chou R, et al. CDC Guideline for Prescribing Opioids for Pain — United States, 2022. MMWR Recomm Rep. 2022;71(RR-3):1–95.https://www.cdc.gov/mmwr/volumes/71/rr/rr7103a1.htm
Cherkin DC, et al. Non-pharmacological interventions for chronic musculoskeletal pain. NCBI PMC. 2002; https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11866493/